Denials are a persistent and significant issue in revenue cycle management, impacting both financial performance and operational efficiency across healthcare organizations. In fact, according to an HFMA survey, the volume of denials from commercial insurers is viewed as the biggest threat to revenue cycles today.
First-pass denials are also on the rise, with rates increasing by 18% from 2020 through 2023. The average first-pass denial rate is approximately 12%, more than twice the industry benchmark.
But not all denials are created equal. Eligibility issues account for more than one in five (21%) denied claims, making them a significant — and preventable — drain on revenue. Every preventable denial adds rework, delays cash and strains staff capacity, each an element that directly erodes financial performance.
Bring denial prevention to the employee level
Most denial prevention programs still center on specific codes. Teams track volumes and dollar amounts at the hospital department level, hoping those trends will point to root causes. While this view highlights where denials occur, it rarely explains why.
Department-level reporting misses the nuanced, front‑line behaviors that drive denials in the first place — things like inconsistent registration workflows, payer‑specific rules or gaps in benefits verification.
Implementing department-level training based on high-level findings rarely results in the behavior changes required to prevent repeated denials. When teams hear overall denial numbers, they often assume the errors belong to someone else, not them, and continue their usual processes. This reflects the bias blind spot, a cognitive bias where individuals tend to rate themselves as ‘better than average.’ As an example, in one study presented in The Economic Journal, 66% of participants rated their own performance ‘above average.’
Without those granular details, leaders can see that there’s a problem but can’t intervene effectively. The result is predictable: pockets of progress, then backslide. Sustainable denial prevention requires deeper visibility into process-level variation so teams can identify true upstream causes, target behavior change and reduce preventable revenue loss. This means that meaningful and lasting improvement requires outreach at the individual level.
Turn precise data into action
Reversing denial trends requires going beyond department‑level dashboards. Ensemble’s approach starts with detailed, individualized reporting that shows how often specific workflows or actions by an employee contributed to preventable denials. Instead of merely tracking aggregate denial counts or dollars, leaders get visibility into the precise denial types and their frequency by employee — a level of nuance that finally makes root‑cause correction possible.
Ensemble integrates directly with EHR data to surface user-level denial volumes and trends based on user-specific fields. For eligibility and registration errors, the system pinpoints the last employee who accessed the registration screens — where critical checks such as insurance verification, coverage dates and eligibility notes should occur.
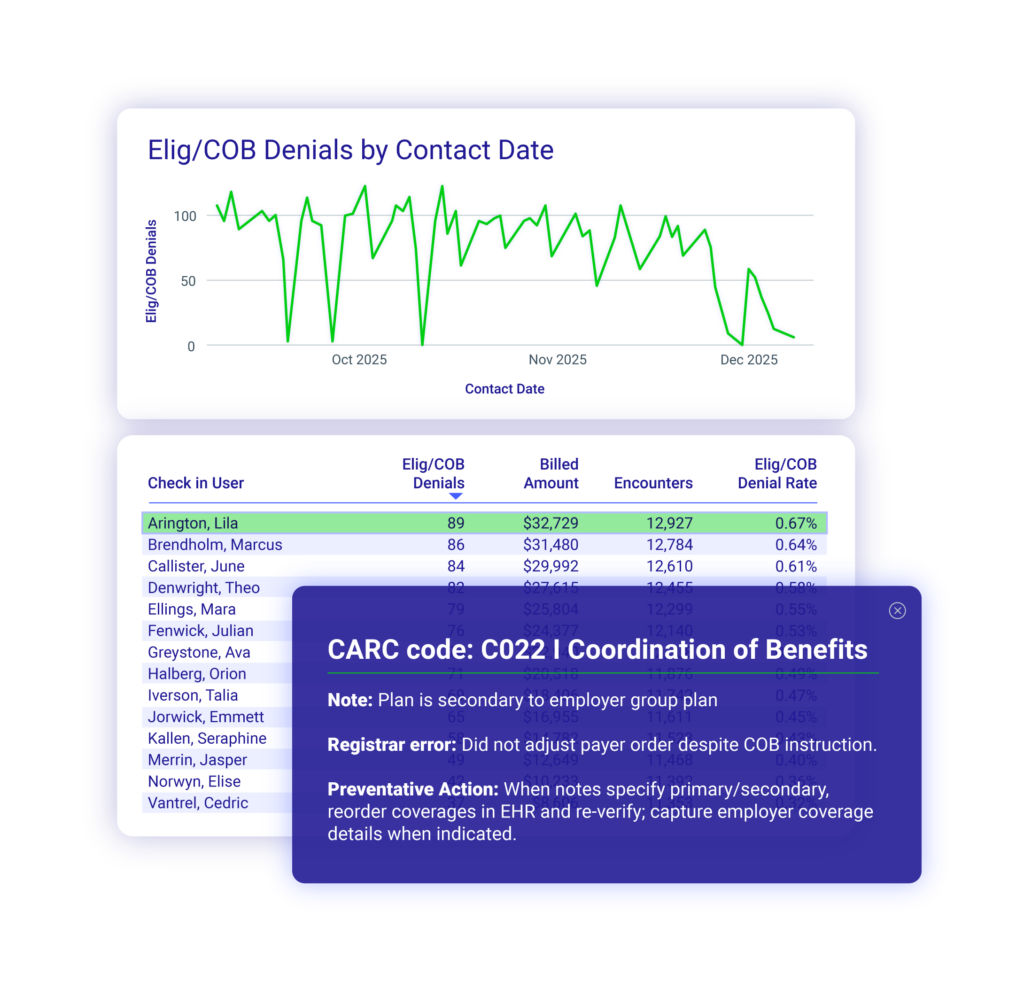
With this clarity, leaders can shift from broad reminders to targeted coaching. Research shows that timely, face‑to‑face feedback is the most effective way to shape lasting behavior change because it reinforces expectations, reduces ambiguity and builds shared accountability.
When leaders use individualized denial data during these discussions, employees understand exactly which steps need adjustment and why it matters for revenue integrity. This creates a practical feedback loop: surface the behavior, discuss it constructively, reinforce training, then measure improvement.
The bottom line
Taking an individualized approach to denial prevention can reduce first-pass denials by nearly 10%. By leveraging precise, user-level data, organizations move beyond department-wide statistics and instead empower leaders to coach employees on the exact behaviors that drive preventable denials. This tailored feedback loop not only addresses root causes but also fosters a culture of accountability and continuous improvement.
As a result, revenue cycle operations become more proactive and resilient, with declining denial rates, stabilized workflows and targeted support for staff. Ultimately, meaningful change and measurable financial benefits come from equipping every employee with the insights and guidance they need to succeed.




