Revenue cycle intelligence
Amplify performance with enterprise AI.
Put big data to work with AI-driven decisioning + advanced analytics.
claims data informing models
best practices
process excellence
and data exchange
Our Approach
AI orchestration across the full revenue cycle
Revenue cycle isn’t solved with a single AI agent. In this video, CEO Judson Ivy explains why it’s critical to build AI that operates as a system, not a stack. Using data from more than 80 million annual claims, Ensemble’s orchestrated AI layer learns, connects and delivers value across the entire rev cycle — from patient access to zero balance.
EIQ: BUSINESS PLATFORM FOR PERFORMANCE
AI that operates as a system, not a fragmented stack.
Our powerful RCM intelligence engine, EIQ®, connects data, people and insights to drive performance across your entire revenue cycle — streamlining operations, uncovering opportunities and integrating seamlessly with your existing systems.
UNIFIED DATA PLATFORM
Power insights and action with data.
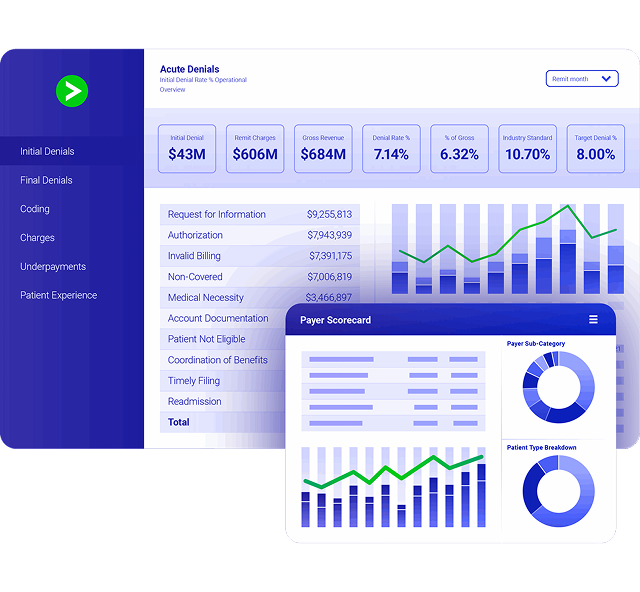
Performance Analytics
Say goodbye to data black boxes.

Revenue performance
Track 100+ metrics from AR aging to cash collections to denial trends — benchmarked against SLAs and industry standards.
Payer insights
Strengthen negotiations and payer performance with scorecards that track underpayments, denial trends and cash velocity.
Patient experience
Monitor satisfaction scores, care access and referral patterns to resolve friction before it impacts care.
Predictive Modeling
Don’t let history repeat itself.
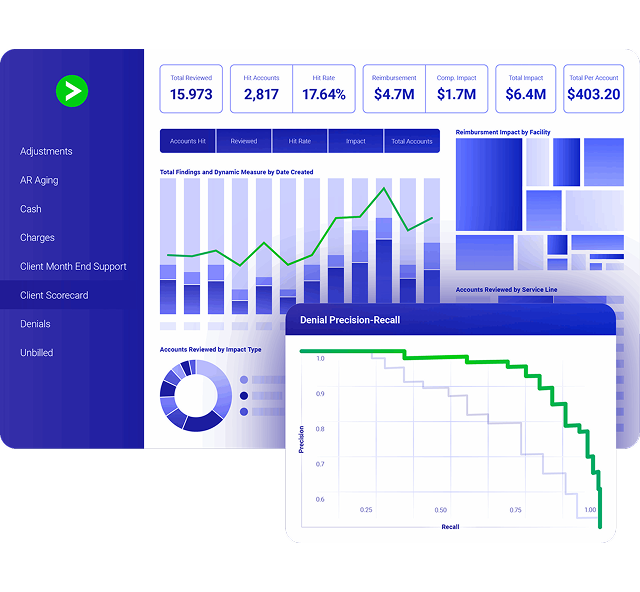
Denial prevention
We analyze 100k+ denial letters to predict risk and trigger early interventions.
Payment anomaly detection
Automated anomaly detection screens every account and flags underpayments and errors in real time.
Tailored patient communication
Anticipate needs and personalize outreach based on patient preferences, historical behavior and account details.


INTEGRATED AGENTS
Replace fragmentation with orchestration.

Conversational AI
Natural language agents securely exchange data with payers and engage patients in HIPAA-compliant conversations.
Operational assistants
From generative denial appeal drafting to real-time call transcription and next best action recommendations, copilots support operators with speed, accuracy and focus.
Agentic orchestrators
Autonomous agents reason, act and resolve to manage complex processes like AR follow-up without human intervention.
IMPACT, DELIVERED
Less friction, better care.
50% reduction in abandoned call rates
by deploying 24/7, personalized, HIPAA-compliant natural voice agents
35% faster call response times
aided by real-time call transcriptions and summaries
40% faster denial appeal submissions
via clinically calibrated generative AI and clinical oversight
92% completion of prior authorizations (eMPA)
with zero manual interventions
100% clinical review success rate
for appeal letters crafted by generative AI
23% more revenue per operator action
with process optimization, AI prioritization and automation
CYBERSECURITY
When it comes to your security, our standards are high.
Ensemble attained a HITRUST r2 certification for EIQ, our proprietary revenue cycle intelligence platform, by demonstrating the highest level of information protection assurance.


TECH SNAPSHOT
EIQ prevents $80 million in revenue loss for health systems in 12 months.
Ensemble’s proprietary revenue cycle intelligence engine, EIQ®, helps hospitals and health systems avoid lost revenue, reduce claim denials and lower administrative costs.
Powered by adaptive machine learning models trained on billions of transactions, EIQ enables pre-bill analysis for 100% of inpatient claims to identify anomalies that traditional human audits often miss. By flagging and addressing errors early, EIQ helps safeguard over $5,000 per account from being lost to inaccuracies, translating into millions of dollars saved across clients.
