As hospitals and health systems continue to face financial headwinds from rapidly rising expenses, workforce challenges and stagnant reimbursement rates, healthcare leaders are turning to their managed care departments as a critical line of defense against avoidable payer pressure.
Historically, market share has dictated authority during contract negotiations between payers and providers, often giving payers the upper hand. So how can providers of any size level the playing field? They must know what provisions to include in their contracts, leverage comparative data to change payer behavior and use price transparency rules to their advantage.
Here are three tips to help improve your next payer contract negotiation.
1. Find the gaps in your current contracts.
Rates are only as good as the payment terms supporting them, so make sure managed care leaders have a strong understanding of existing contract terms as well as the best practice language required to drive proper reimbursement.
For example, do you have provisions that require the payer to pay, deny or dispute a claim within 30 days or remit payment with interest on day 31? Are you preventing pre-payment review on claims not disputed within 30 days? How are you limiting requests for information, audit volumes and appeal response timelines? Are you restricting bundling of charges and limiting “lessor of” language? How are you protecting yourself against recoupments?
Tracking and maintaining a list of managed care contract provisions and recommendations gives providers a path to increase reimbursement rates and ease costly administrative burdens.
2. Compare payer performance.
Make sure you’re tracking and comparing payer trends across your organization. Build a payer scorecard to analyze performance across your commercial payers and identify trends that need to be addressed during your next negotiation. Focus on metrics like clean claim rate, payment as a percent of charges, denial rates and reasons, underpayments, appeal volumes and win rates and other year-over-year net reimbursement changes.
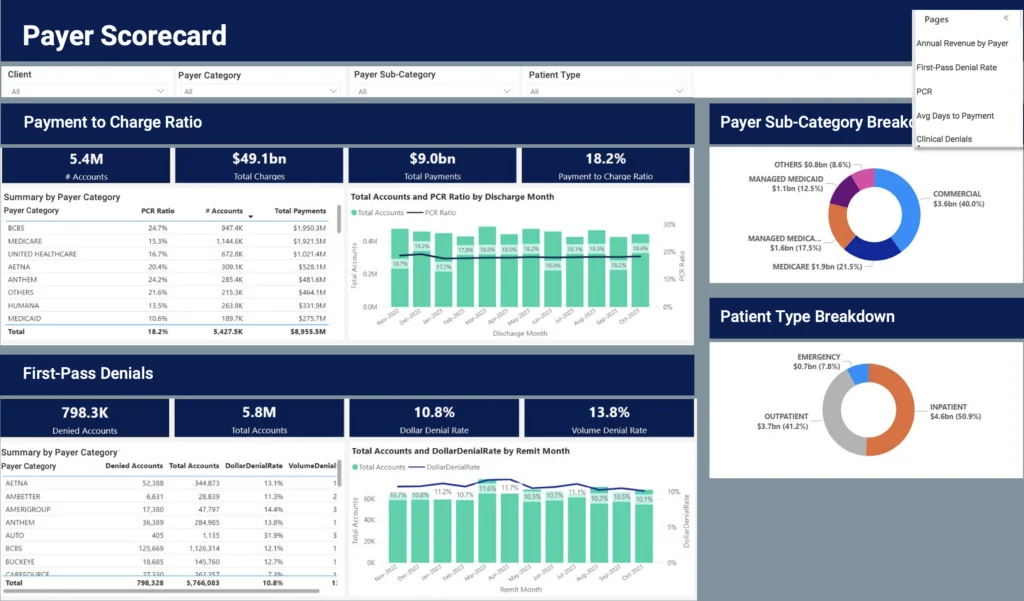
Showing the total revenue impact of a payer’s behavior and comparing trends with other payers can help influence negotiations and accelerate issue resolution.
3. Use payer price transparency requirements to your advantage.
Research and download corresponding in-network rates for each commercial payer with an upcoming negotiation. The size and scale of the available machine-readable files makes this a labor-intensive project, so create a project plan with enough lead time to download and review potentially thousands of files.
Compare your existing contracted rates with publicly available rates for the same payer across other providers. Look for any large variances between what your facility is paid and what other facilities in your geographic area have contracted for. Focus on high-dollar procedures, items and services, especially those aligned with the unique specialties or credentials of your organization. Consider current and expected patient volumes to accurately estimate the revenue impact of any current rate discrepancies or future adjustments.
And don’t overlook out-of-network payers. Review their payment rates and examine the revenue impact of bringing an out-of-network payor into your network.
Key Takeaways
With razor-thin operating margins, healthcare providers can’t afford to lose precious revenue due to unfavorable contract terms, inadequate protections or unknown contract loopholes. Ensure your organization has a strong managed care team equipped with the necessary data, contract language and negotiating strategy to even the playing field between you and your commercial payers so your organization can improve financial health and continue to navigate industry headwinds.
____
Andrew Bess leads Ensemble Health Partners’ payer strategy team, helping healthcare clients across the U.S. improve managed care strategies, negotiate favorable payer contracts, analyze national payer trends and successfully resolve issues by working side-by-side with national payers.
These materials are for general informational purposes only. These materials do not, and are not intended to, constitute legal or compliance advice, and you should not act or refrain from acting based on any information provided in these materials. Neither Ensemble Health Partners, nor any of its employees, are your lawyers. Please consult with your own legal counsel or compliance professional regarding specific legal or compliance questions you have.

